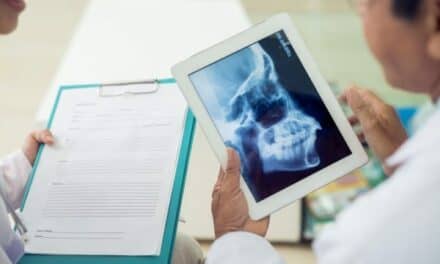
New technology is enabling continuous monitoring of all vital signs, even for non-ICU patients. That means earlier detection and intervention when a patient is in trouble, leading to increased patient safety
The data is clear: On average, 50% of hospital deaths occur in the unmonitored patient population.1 Despite increasingly widespread use of sensors to monitor vital signs and physical activities of healthy individuals, the majority of acutely ill hospitalized patients remain unmonitored, leaving them at risk.
Increasingly, hospitals are charged with treating sicker patient populations, even outside the ICU. Comorbidities (the simultaneous presence of two conditions in a patient), complex pharmaceuticals, and unpredictable or unknown risk factors are common in non-ICU patients, leading to more fluctuations in their health status. Within this environment, patient deterioration can go unrecognized, resulting in adverse events or worse. This failure to detect is particularly troubling given that most patients who experience decline show evidence of deterioration for as many as 6 to 12 hours prior to their clinical event.2,3,4
Part of the problem is that today’s standard for nursing rounds and vital sign measurement has not kept pace with the increasing acuity of hospitalized patients, which may make them more susceptible to changes in condition. This lack of modernization in patient observation methods is especially apparent in densely populated, lower-acuity areas of the hospital, where physiological assessment is typically performed only every 4 to 8 hours. In many facilities, no system focuses on protecting general-ward patients who are not under direct observation.
With the rise of new patient monitoring technology, there is increasing interest in new approaches, such as surveillance monitoring of hospitalized patients who are not traditionally monitored. Whereas conventional condition monitoring focuses on patients identified as being at risk for problems (for instance, a patient with known cardiac disease is placed on telemetry), surveillance monitoring encompasses patients who have not been identified as being at specific risk. This approach is intended to increase safety, enhance quality of care, and improve workflow.
This article focuses on the call for continuous, multiparameter patient surveillance monitoring of all vital signs in general care areas as a new standard of care; the requirements of an effective surveillance monitoring system; and potential benefits and deployment considerations.
Recognition, Reporting, and Responding
The fundamental assumption of surveillance monitoring is that early identification of deteriorating patients will improve patient safety. This can occur in two ways: by identifying deterioration and stabilizing patients on their existing ward, or by expediting transfer of patients to more appropriate levels of care.
In 2010, a report from an international consensus conference on rapid response emphasized the need to concentrate on a rapid response system (RRS) that can detect when a patient is at risk and trigger a call for assistance, while also facilitating collection of data for administrative and data analysis. The report cited studies that have repeatedly revealed widespread shortcomings in how hospitals typically acquire and act upon abnormal vital signs. These errors must be overcome in order to improve failure to rescue statistics.5
Successful rescue of a patient requires three criteria: recognition that the patient requires acute intervention, reporting that knowledge to appropriate personnel, and an effective response. Failure in any of these areas will lead to failure to rescue.
Surveillance monitoring is key to recognizing and reporting physiological instability. As the consensus conference noted, a defined a set of core vital signs should always be monitored: heart rate, blood pressure, respiratory rate, temperature, pulse oximetry, and level of consciousness. The group agreed that “if practical and affordable, all patients should be monitored continuously.”1
A New Standard of Care
In response to evidence documenting the need for more effective monitoring tools, continuous, multiparameter surveillance monitoring is emerging as a new standard of care for the general medical/surgical population. The use of continuous vital sign monitoring systems in the general care setting offers a more proactive approach to identifying patient deterioration. The shift is based upon a simple premise—that a patient’s physiologic changes can indicate, and perhaps predict, deterioration episodes before they occur.
The quest to develop systems that can be used outside of the ICU to detect patient deterioration prior to an event has become a kind of holy grail, and the subject of intense study. The 2010 report from the international consensus conference on rapid response systems listed the desirable characteristics of an effective surveillance monitoring system. Today, few systems align with these comprehensive requirements, noted in Table 1.5
While cardiac telemetry systems would appear to fulfill these needs, current systems do not address the complete set of core vital signs recommended for monitoring by the rapid response experts and significantly hinder mobility. However, wearable surveillance monitoring systems enable freedom of movement and allow clinicians to keep tabs on their patients at any time, from any location. Worn on the body, these systems enable continuous monitoring of all vital signs and communicate wirelessly with a patient’s electronic health record. The systems can also be customized with novel alarm analytics to reduce disruptions and promote safety.
Benefits of Surveillance Monitoring
The adoption of continuous surveillance monitoring of all patients is a patient safety investment that can provide several tangible benefits. For instance, hospitals that have placed patients in the ICU simply to provide a higher level of surveillance can now be transferred to a lower-cost-of-care setting and still receive continuous monitoring of all vital signs.
Likewise, in cases where the emergency department (ED) is experiencing a bottleneck processing patient admissions due to a shortage of available telemetry beds, patients can be admitted to a general ward that provides continuous surveillance monitoring. This approach could free up ED beds and improve the availability of real-time information about the patient’s condition.
Surveillance monitoring technology can also serve as a tool for demonstrating best practices. Data on specific events can be used to assess clinical practices and clinical outcomes. Vital sign measurements can also be correlated with other data (such as level of consciousness) for trend analysis or integration into electronic health record-based Early Warning Scores.
Detecting early signs of patient deterioration plays an important role in improving a hospital’s clinical, operational, and financial performance. Data analysis can help organizations identify accurate markers of deterioration, so that clinicians can be notified proactively within the context of normal care delivery.
Although it is too early to evaluate patient attitudes toward surveillance monitoring on a large-scale basis, anecdotal evidence is promising. Patients and their families generally view the technology positively because of its ability to enable improved mobility and a more restful environment.
The Issue of Alarms
For continuous surveillance monitoring of all vital signs to be effective, and ultimately adopted into nursing practice, the system needs to detect patients at risk while not adding to a facility’s alarm burden. The system must identify true, actionable events with high sensitivity, avoiding false alarms while also supporting patient mobility.
High-acuity monitoring systems do not meet any of these criteria, and as a result have not been broadly adopted for use in surveillance monitoring. In many general care units, the burden of too many nuisance alarms associated with those systems outweighs the nursing benefit of continuous monitoring.
When determining alarm and alert strategies for surveillance monitoring, healthcare organizations should consider these fundamental questions: Why is the patient being monitored? What are the primary goals of surveillance? Is monitoring intended to be primarily predictive (anticipating deterioration before it occurs), detective (identifying deterioration as it occurs), or both?
It is recommended that facilities begin with detection monitoring, the least complex of these options. In “detective mode,” surveillance monitoring serves as an ongoing diagnostic test that continuously assesses the patient for the emergence of new clinical states (the recognition phase).
However, finding the right ratio of alarm sensitivity to specificity can be a complicated process. If alarm thresholds are set too liberally, the monitoring may be overly sensitive and generate a high level of nonactionable alerts that can contribute to alert fatigue. Since many physiological alerts are self-correcting, introducing alarm delays may help improve specificity. But if delays are too short, specificity will suffer and again result in excessive nonactionable alerts.
So what is the best approach to establishing alarms, alerts, and alert-delay thresholds? One approach is to use data analytics and customized tools to run evidence-based simulations. Such tools allow hospitals to predict, based upon their own set of alarm thresholds, what subsequent alert volumes will be, enabling a very tailored approach to setting alarm sensitivity and specificity.
At first, some clinicians may consider the resulting alert parameters extreme or risky, since they are likely to be very different from what clinicians have used in the past. However, it is important to recognize that because alerts will sound infrequently, the information should have a high degree of actionability, thus minimizing the problem of alert fatigue. As use of the system progresses, alarm settings can be further refined with the institution’s own data.
Finally, a common source of false alarms is motion artifact (for example, spikes or dips caused by normal bodily movement rather than a change in condition). Reducing these alarms is critical to a positive outcome, particularly for a population of patients that is likely to be mobile. Safeguards that offset the effects of motion artifact can contain nonactionable alarms and help ensure a successful surveillance monitoring system.
Deploying A System
The move to a continuous surveillance monitoring system represents a significant leap forward in quality and care for a healthcare organization. It requires not only adaptation to new equipment, but also full acceptance of a new clinical workflow. To realize the full potential of such an investment within a reasonable timeframe requires commitment on the part of both the hospital and its vendor. The two must work together to define the clinical environment, establish desired workflow, and determine the key success factors to be applied. They must also collaborate to allocate resources, engage stakeholders, and meet all clinical, organizational, and technical needs.
A cohesive team is at the center of a successful implementation. The hospital task force should include a key executive, physician and nurse representatives, the clinicians who will be involved in training employees, and technical leads for equipment installation and information system management. It is also helpful to involve a clinical educator when devising the training protocol.
For the clinical team, preparation focuses on promoting an understanding of the project’s clinical objectives and training staff on new workflow procedures. Surveillance monitoring systems can present numerous configuration options: parameters that must be considered include alarm limit thresholds, units of measure, unit room/bed configuration, and other settings. The team must work together to define a clinical configuration that will meet the hospital’s needs.
A successful deployment should also involve the development of a policies and procedures document. These guidelines should specify required competencies in the use of the system and identify which patients will be monitored and for how long. They should also include detailed roles and responsibilities for the staff that oversee the system, the proper procedure for alarm response, and the policy for customizing alarm limits.
To initiate technical implementation, the vendor should perform a wireless network assessment to ensure that the hospital’s target deployment areas have the necessary wireless coverage for optimal performance. The assessment should also include spot checks to collect data on interference, bandwidth utilization, retries, and other statistics pertinent to a successful deployment.
Interoperability is another factor for facilities to consider when deploying a continuous monitoring system, since it is often crucial to maximizing the platform’s potential. Three potential levels of interoperability will improve the system’s effectiveness. Admission-discharge-transfer (ADT) integration allows the hospital’s patient demographic information to be used for patient association. Integrating the system with the electronic medical record (EMR) enables automatic vital sign capture, which increases the speed and efficiency of clinical workflow and reduces errors associated with manual transcription. (Clinicians must still regularly review the vitals captured in a patient’s chart.) Integrating the monitoring system with clinician’s mobile devices can achieve a third layer of interoperability by providing alarms directly to the care providers.
Effectively leveraging a continuous multiparameter patient monitoring system to reduce failure to rescue and failure to respond statistics depends on an optimized alarm configuration. During the implementation process, hospitals should undertake a comprehensive analysis of their current alarms and analyze possible alarm configurations to balance the benefit of their individual alarm configurations against the burden placed on nursing staff. By adjusting threshold levels and alarm delays, they can then measure outcomes to determine whether the changes result in any missed events.
An Important Safeguard
No nurse should enter a room and unexpectedly find a patient in extremis, or worse. Surveillance monitoring provides an important safeguard, protecting patients when the nurse is not in the room to prevent such a catastrophe from happening.
Surveillance monitoring represents a critical opportunity to improve the delivery of high-quality, safe, effective healthcare. With multiparameter continuous monitoring, it is now possible to improve recognition and reporting of physiological deterioration. Hospital resources can therefore be leveraged earlier and more effectively, saving money and lives.
James Welch is executive vice president of product development at Sotera Wireless in San Diego. For more information, contact chief editor Jenny Lower at [email protected].
References
1. Haraden C. Diagnostics for Patient Safety and Quality of Care. Patient Safety Executive Development Forum, Institute for Healthcare Improvement. Retrieved November 13, 2014 from http://www.ihi.org/education/conferences/APACForum2012/Documents/I2_Presentation_Diagnostics_Haraden.pdf.
2. Schein RM et al. Clinical antecedents to in-hospital cardiopulmonary arrest. Chest. 1990;98:1388-92.
3. Hillman KM et al. Duration of life-threatening antecedents prior to intensive care admission. Intensive Care Med. 2002;28:1629-34.
4. Buist MD et al. Recognising clinical instability in hospital patients before cardiac arrest or unplanned admission to intensive care. A pilot study in a tertiary-care hospital. Med J Aust. 1999;171:22-5.
5. DeVita MA et al. “Identifying the hospitalized patient in crisis” — A consensus conference on the afferent limb of Rapid Response Systems. Resuscitation 2010;81(4):375-82.
Photo credit: Sotera Wireless