 |
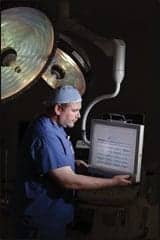
| Phillip Knecht, senior technician, clinical engineering, Southeastern Regional Medical Center. |
Small departments often have modest resources, but they are still responsible for big workloads. With three technicians—two in charge of repairs and one who concentrates on preventive maintenance (PM)—the clinical engineering team at Southeastern Regional Medical Center in Lumberton, NC, fits this profile perfectly.
Southeastern serves more than 71,000 patients in its emergency department and more than 15,000 in-patients. The 337-bed hospital also operates a 115-bed long-term care center and offers a wide array of health care services through its affiliated divisions. The biomedical/clinical engineering department is responsible for these facilities’ growing inventory, presently at 6,000 devices, few of which have service contracts. When a piece of equipment cannot be found or work orders go missing, significant time, productivity, and, subsequently, dollars are also lost.
While more help is appreciated, new hires are not always the answer. Sometimes, the more robust solution is technological. Digital systems that match a department’s needs can help to manage workloads, track inventories, and improve efficiency, adding value that extends past an extra pair of hands (and sometimes two or three). Southeastern long ago recognized the value of both computerized maintenance management systems (CMMS) and real time location systems (RTLS), but could not find the software or system that matched its needs. In 2007, that changed, and last year, the health care institution installed one of each—the CMMS in April and the RTLS in December.
Despite the hectic environment created by two major implementations so close together, the estimated return on investment (ROI) made both projects self-evident. For instance, Phillip Knecht, senior technician in Southeastern’s clinical engineering department, notes the RTLS estimation took into account the volume of “missing” equipment, the associated cost, and the time spent attempting to locate it. Once the math was done, buy-in was captured.
Now that the installations are complete, the clinical engineering department is beginning to quantify the results and calculate the returns. Yet, even without enough time to evaluate postinstallation data, the improvements in workflow and cost efficiency are already evident.
COMPUTERIZING INVENTORY AND MAINTENANCE
Senior BMET Richard Wheeler recalls that before the CMMS implementation, clinical department staff would stop him and give him oral work orders as he walked to a scheduled repair or PM. Not surprisingly, some orders were forgotten along the way. When not forgotten, obtaining the needed information was hindered by inefficiencies, such as phone tag.
Orders that were called in were often messages mentioning the department and the device type; callers did not always identify the specific device or even themselves. “We’d go looking for it and never find it,” Knecht says. The system was inefficient and resulted in angry callers asking about work orders that had been “placed” weeks ago. Digital work orders have eliminated those frustrations.
“Now, we actually have work orders,” Wheeler says. Using the new work order center, clinical staff create and track work orders, and the clinical engineering staff receive them immediately, even if remote. The system Southeastern selected, TMS Enterprise from Four Rivers Software Systems, Pittsburgh, offers a module for mobile connectivity so work orders can be accessed wirelessly via PDAs or BlackBerries.
 |
 |
 |
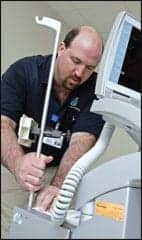
| RTLS benefits include full facility coverage, scalability, and improved patient care. Here, Senior BMET Richard Wheeler tests a balloon pump and places an asset tracking tag on the device. | ||
The work orders can also be printed and affixed to broken equipment to serve as notice. “So if a staff member comes up to use the device, they can see a work order has already been placed,” Wheeler says. “They don’t waste time trying to use it or calling in another work order.”
In addition, the information needed to complete a work order is actually complete—mandatory fields in the electronic document ensure it. These include the asset tag number, a brief description of the problem, the name of the reporting employee, and his or her contact information.
LOCATING SYSTEMS
To be sure the system would work, Southeastern negotiated a trial. “You want to take some of your information and enter it in the new system so you can look at what you know,” Wheeler advises. He suggests it is one of the best ways to avoid purchasing something that does not fit.
Biomedical/clinical engineering departments also want to evaluate more than one system. “You’ve got to take what everyone has, evaluate it, and see which one will work best for you,” Wheeler says. And if something does not work, then it is OK to pass.
Southeastern delayed purchasing an RTLS system for years until it found one that could meet its needs without exceeding its budget. “We recognized the necessity of an asset tracking system and began our search several years ago,” says Charles Brady, NICET, ASCET, NARTE, director of clinical engineering at Southeastern. “At that time, the systems available did not achieve results that justified their prohibitive cost.”
But times change, and eventually Southeastern looked closely at two companies before selecting a system from RadarFind Corp, Morrisville, NC. “We needed a system that was easy to install, nondisruptive to hospital operations, gave accurate, reliable locations, and could give us hard direct data on our utilization of devices,” Knecht says. His tip: “Look for a company that can do the install [turnkey] without interrupting biomed or IT.”
Additional advantages included full facility coverage, scalability, a lack of interference with other hospital systems, and a low total cost of ownership.
The purchase was approved in December 2007, and installation began in March 2008. Administration buy-in was secured with the projected improvements in patient care. “Our CEO, Joann Anderson, was highly in favor of purchasing the system,” Brady says. “Being able to locate equipment to give quicker service to patients is the main advantage.”
 |
| Senior BMET Richard Wheeler keys information into the RadarFind database to track assets. |
Knecht notes they are well on their way to hitting some of the project’s objectives. These goals include “reducing capital equipment expenditures by right sizing the hospital’s mobile medical device inventory, increasing the hospital’s operational efficiency, and ultimately improving patient care and satisfaction,” Knecht says.
Employee satisfaction across departments, such as nursing, clinical engineering, and materials management, was another expected benefit. “Before RTLS,” Knecht recalls, “we would have to walk through the hospital and look for the devices, trying to find even those that were stored in closets or left in out-of-the-way places. That was very time-consuming and somewhat frustrating.” And Knecht was not the only one frustrated by wasting time—often overtime—looking for lost devices.
“At any given time we could not account for about 10% of our inventory,” says David Sumner, vice president of strategic management and support services for Southeastern, in a release addressing the RTLS installation. “We were spending time and resources to track IV pumps, stretchers, wheelchairs, and mobile monitors. It was not unusual to realize that when we inventoried our wheelchairs, close to 90% were unaccounted for.”
POSITIONING THE RTLS
The RTLS solution was simple, and the installation was smooth. The system components include tags, readers, collectors, and software. RadarFind offers tracking devices for both assets and patients, though Southeastern is currently only tracking equipment.
The footprint has been minimal. The tags easily attach to equipment and communicate with readers that plug into electrical outlets. “Basically, we put the readers in hallways and every other patient room. We currently have 290 readers in-house,” Knecht says.
Though the readers are located in existing electrical outlets, they do not disrupt the outlets’ function. They required neither new wiring nor wall penetration, and the installation created “virtually no disruption,” Knecht says. During installation, patients, for instance, were able to remain in place.
Currently, Knecht estimates South-eastern is tracking about 750 devices, and the list continues to grow. Instruments already in the RTLS system include beds, BP/vital signs monitors, dialysis machines, EKG/defibrillation devices, feeding pumps, infusion pumps, mobile carts, PCA [patient-controlled analgesia] pumps, ventilators, sequential compression devices (SCDs), ultrasound/Doppler, wheelchairs, and stretchers.
Knecht approached the conversion by starting with the most in-demand items: infusion pumps, SCDs, wheelchairs, and BP/vital signs monitors. By choosing these items, Knecht believes “you can have the most impact on the greatest number of people in the shortest period of time.” As the RTLS inventory expands, the hospital can add readers and tags as needed.
Some items will never be added to the system. Items that are fixed, such as wall-mounted monitors, do not typically need tracking. The general rule of thumb, according to Brady, is if the device moves and RTLS can help staff find it easier, “then you probably need to track it.”
Because so many devices and personnel are involved, naming conventions are important. One of the bigger challenges in implementing an RTLS was rethinking the organization of the hospital’s asset list and the classification of clinical areas and equipment common to all user groups, not just the engineering staff.
“In order for there to be uniformity throughout the system, there needs to be strict adherence to a consistent and logical device-categorization hierarchy,” Knecht says. “We have followed the RadarFind system that allows the location of any device within three to four clicks using their user interface. There is a simple lexicon used that is easily recognizable for the end users, like nursing transport and central sterile.”
Wheeler explains the process using infusion pumps. “We have five different kinds of infusion pumps in our hospital. There are large volume infusion pumps, syringe pumps, PCA pumps, feeding pumps, and epidural pumps,” he says. All of these pumps are included under the broad umbrella categorization of infusion pumps. When this category is selected, the user then has the subcategories of pump type as options. “This allows you to choose the type of pump you need to locate without having to look through the complete inventory of infusion pumps,” Wheeler says.
INTEGRATING THE SYSTEMS
The system is easily accessed through the hospital Intranet. A link on the site provides anyone with read-only access. “I use the system often throughout the day,” Wheeler says.
Eventually, the RTLS system will be integrated with the CMMS. “We are developing integration protocols for our existing scheduling and inventory software, but the integration is in the beginning stages and I do not have a time line,” Knecht says. However, RadarFind has been flexible in making modifications to accommodate the hospital’s unique needs, including the integration.
For instance, a newly developed search engine was created to offer clinical staff the ability to look for specific devices within the RTLS. “The equipment in our hospital is owned by each department and is inventoried to reflect this ownership,” Knecht says. “When equipment is borrowed by another department, we have found that the original owners can locate it easily by checking the RadarFind system.”
However, Knecht adds that Southeastern also hopes “to see a greater sense of shared assets throughout the hospital rather than a sense of individual ownership that comes from not being able to locate things when you need them.” With instruments easily found, there is less tension surrounding their use.
Biomeds often use the system to complete their work orders, particularly PM. “One of the most important aspects of our job is preventive maintenance of all hospital medical equipment that is used in patient care,” Knecht says. “There is an enormous amount of individual items, most of which are checked at least once a year, many of which randomly move constantly throughout the hospital in their role of supporting patient care. Some devices need to be maintained multiple times per year.”
 |
| L-R: Samuel (Wally) Jackson, BMET I, and Senior BMET Richard Wheeler test an infusion pump. |
Like many other clinical engineering departments, Southeastern has established a schedule to ensure that PMs are performed on a particular category of devices within the established time frame established by the manufacturer and regulatory guidelines. “The pressure is to find every device within the prescribed time period and maintain the schedule,” Knecht says.
Before RTLS, the task was time consuming and wasteful. Now, the system is the central tool in the department’s efforts. “My workflow has been more streamlined,” Wheeler says. “Now, instead of looking all over the hospital for equipment for PM, I go to RadarFind and key in the control number of the equipment I am looking for. It shows me the exact location of the equipment.”
He notes he uses it primarily to locate PMs, but will also search for equipment with a repair work order that was not where it should have been. Tagged items are located quickly, and their status is easily determined. The tags also feature a status change indicator. The three default positions are “available,” “in use,” and “needs cleaning.”
Brady notes that the PM rates have already improved with the installation of the RTLS. “Once all equipment is tagged with tracking tags, then PM completion rates should be 100%,” he predicts.
PROFITING WITH SOFTWARE
Along with the increase in productivity, the hospital expects to see costs decrease in a number of areas, not all of them fully understood. “The full impact on workflow in other areas has not been fully delineated,” Knecht says. But the RTLS tracks and mates devices that are essential to almost all departments throughout the hospital, including the ORs, transport, outpatient procedures, respiratory therapy, physical therapy, and nursing in general.”
|
Read more about RFID in the January Service Solutions article. |
One obvious reduction is in overtime, which in the past was often needed to track lost materials. Now that time can be better spent, if it needs to be spent at all. ROI, however, is not measured solely in productivity and satisfaction. The smart use of both the CMMS and RTLS can also reduce expenditures on equipment. With devices easily tracked, there is no longer a need for excess inventory to replace “missing” items.
It is too soon for Southeastern to have final financial data, but when the calculations are complete, it is likely the ROI estimations will have been met. Knecht already describes the rewards for the small department as “tremendous.”
Renee Diiulio is a contributing writer for 24×7. For more information, contact .
REFERENCE
- Van der Rogt R, van Lieshout EJ, Hensbroek R, et al. Electromagnetic interference from radio frequency identification inducing potentially hazardous incidents in critical care medical equipment. JAMA. 2008;299(24):2884-2890.
 |
NO INTERFERENCE WITH PROGRESS
In June 2008, the Journal of the American Medical Association (JAMA) published a study that found “in a controlled nonclinical setting, RFID induced potentially hazardous incidents in medical devices.”1 The researchers recommended that institutions implementing the tracking technology conduct on-site electromagnetic interference testing. Debate immediately ensued.
Much of the controversy surrounds the actual technology. Many vendors offering real time location systems (RTLS) have developed technologies that eliminate interference problems. The JAMA study researchers used two RFID systems operating in the active 125-kHz and passive 868-MHz ranges. Many RTLS vendors use less powerful frequencies in different ranges. For many, the technology is not even technically “RFID.” Technologies, such as Wi-Fi, ultra wideband (UWB), and ZigBee, are often referred to as RFID, but, according to standards, they are not actually RFID technology.
RadarFind Corp, Morrisville, NC, stated in its response to the study that, “While some RTLS technologies are related to RFID in that the system components are architecturally similar, the two terms are commonly and mistakenly interchanged.” RadarFind’s RTLS tags operate in the 900-MHz to 928-MHz range specifically to avoid interference with clinical equipment. Its readers use far less power than those in the JAMA study—about 20,000 times less, according to the company.
Phillip Knecht, senior technician, clinical engineering, Southeastern Regional Medical Center, Lumberton, NC, reports that its use of RTLS has not resulted in any interference with clinical equipment in the hospital. “The power levels and frequencies designed into the RadarFind system were idealized for the health care environment, and interference has not been an issue,” he says.
Even though many RTLS developers have eliminated interference concerns, buyers should always consider the issue and discuss it with potential vendors. Evaluation should include understanding the system’s power emission and its characteristics, the spatial environment in which it will be used, and the clinical equipment in that environment. Installation should include performance testing to be certain of interference-free use. Further studies may show that interference is a thing of the past, but either way, RTLS appears to be a way of the future.
—RD