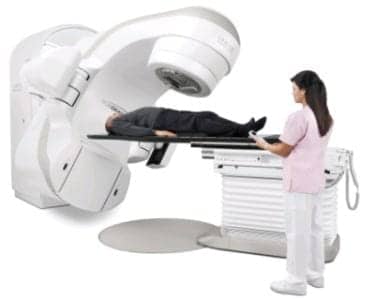
Linacs deliver external beam radiation treatments to cancer patients. Photos courtesy of Varian Medical Systems.
Linear accelerators, or linacs, are large, complex, expensive devices. They are also very active, useful, efficient machines. Generally, they deliver external beam radiation treatments to cancer patients, but they may also incorporate additional systems to provide them with specific capabilities.
“These machines are not just linear accelerators anymore,” says Alex Perec, senior imaging engineer at the University of Rochester Medical Center (URMC) in Rochester, NY. “They have imaging systems attached to them, such as portal dosimetry or onboard imaging systems, and these add to the complexity of the machine.”
It is, therefore, imperative for any clinical/biomedical engineer who works on these machines to understand what it is these machines do. “You can’t walk into these green. Even if you have the training, you’re still not going to be effective at it until you have some hands-on experience,” says Don S. DiVita, URMC’s clinical engineering director.
The investment in this expertise can be expensive and should be a serious factor for any department considering bringing a greater portion of the service and maintenance of these devices in-house. This consideration will make up a significant portion of the expense side of the equation.
The other side of the formula includes savings in downtime that can impact not only the revenue generated by the activity on the machines, but the care delivered to patients—an intangible figure. “Patients can only miss so many treatments because of the cumulative effect of the radiation on the cancer cells,” DiVita says. “If you stop treatment, you have to start all over again. So it’s critical that patients get their treatments on a regular basis.”
Understanding Linacs
Linacs treat patients with targeted beams of high-energy x-rays. Based on principles first developed by the Norwegian Rolf Wideröe in 1928, linacs are essentially particle accelerators that harness the energy generated to kill tumor cells. The technicians can focus the beam to pinpoint the cancer cells and spare the healthy surrounding tissue.
The treatments can be applied anywhere throughout the body with applications that include intensity-modulated radiation therapy (IMRT), image-guided radiation therapy (IGRT), stereotactic radiosurgery (SRS), and stereotactic body radiotherapy (SBRT).
Complex algorithms incorporating mathematics and computer modeling are used to plan these treatments. Data includes imaging results that indicate the depth and placement of tumors so that appropriate levels and directions are applied to the radiating beam. “What clinical engineering does is maintain the systems that produce the radiation used to treat the patient,” DiVita says.
To do this, clinical/biomedical engineers need to understand what the systems do and the purpose of their use as it will facilitate troubleshooting. “If you don’t understand the problem being described, it’s far more difficult to diagnose and repair [the machine],” says Wally Elliott, CCE, clinical engineer with instrumentation & technical services (ITS), University of Vermont (UVM), Burlington. Sometimes, the problems can be very subtle, so it takes an understanding of the therapy to be able to translate that issue into what might be happening with the hardware or software.”
Service Costs and Challenges

Maintenance is often done off-hours,
raising in-house labor costs.
Developing this understanding, however, takes significant time and investment. Some of the subtler issues cannot be easily taught or are not readily encountered. “It takes more than sitting in on a couple of treatments,” Elliott says.
Typically, the individuals who work on linacs within a hospital system or other facility are the highest-level biomeds or clinical engineers employed within the institution. This means they will include the highest-paid individuals in the department who will attend some of the most expensive (and lengthier) vendor service schools. DiVita estimates linac training can run anywhere from $20,000 to $30,000. Depending on the level of expertise, it could run higher.
“The linac portion of training is about 6 weeks of school over a 2-year period,” Elliott says. “Then you could go to school for the onboard imaging system. The MLC [multileaf collimator] could be a different school.”
The process could take 3 to 4 years in its entirety, hands-on expertise included. Manufacturer representatives will automatically attend every relevant school. “We have to decide how much we can afford,” Elliott says.
Initial training is often included with the purchase of a system, but it does not apply to new staff members, whether they are additional or replacement staff. Because of the expense, these training dollars are often spent carefully.
“It’s not your basic entry level,” DiVita says. “Before I allow an engineer to service a linac, they have to go to service school or work with an engineer who has gone to the service school. And before I send them to service school, they have to be a high-level and experienced employee.”
If the expertise does not exist in-house, it may be possible to recruit an experienced individual or work with the vendor while the experience is developed. Departments with in-house programs will often create backup plans and start less experienced personnel on specific problems to help them get a feel for the machines. “If you have more than one person in-house, it’s helpful to work as a team to develop that experience,” Elliot says, noting he and another staff member handle linacs for ITS at UVM.
When Things Go Wrong
The experience is key because the machines are so complicated and involve a large number of subsystems. There is generally a particle source, a high-voltage source, a hollow pipe vacuum chamber, a radiofrequency energy generator, air pneumatic systems, water systems, onboard systems, and many mechanical parts.
“You need an individual who is good mechanically and electronically,” says Brian Wallace, radiation therapy service specialist with the clinical engineering department of St Vincent Hospital in Green Bay, Wis, an affiliate of Hospital Sisters Health System.
Because there are so many systems and parts, there are lots of opportunities for failure. With a typical treatment tolerance limited to a millimeter, there is not a lot of room for error. “People drop hand controls. Motors blow up. High-voltage sections and computers fail. There are all types of different things that can cause the system to be down,” says Bill Vidro, imaging team leader on the URMC team.
No system is problem-free, but those that are more mechanical tend to see more problems. “The mechanical parts cause the most issues and physically break down over time,” Wallace says. However, repair is not always a simple swap—the radiation component complicates matters further.
“It’s not something that comes intuitively to technicians because we’re so used to replacing components with what we perceive as equivalents, but these might not be equivalents in a high-radiation environment,” Elliott says. Some parts will be more affected by radiation than others.
“During a repair or preventive maintenance, you have to question which lubricants, hoses, cables, and even tie-wraps you use,” Elliott says. “Some of them are affected by the radiation; others less so. So it’s not something that you just start doing without having some direction or assistance.”
Parts are checked during PMs, and if a failure seems imminent, they can be replaced preventively. PMs are generally recommended by the manufacturer three to four times a year and involve extensive checklists. The machines also typically have onboard alert programs that shut the device off if a problem is noted. “There is redundancy built in as a safety measure,” Perec says.
Where to Find the Time
Safety features help to protect patients and technicians and are key to otherwise incredibly busy machines. In many facilities, a patient is scheduled every 15 minutes throughout the day, for 8 hours (or so, pending the facility schedule), 5 days a week. Because of the importance in meeting treatment delivery schedules, sites are loathe to give up the machine.
“If the technicians or therapists can bypass the issue, still treat patients, and limp along through the day, they will do so in order to get all the patients treated on time,” Wallace says. This continued use does not negatively impact the performance of the device or the severity of the problem, but it does mean obtaining access to these machines can be extremely difficult and, in fact, is often cited as one of the biggest challenges in servicing and maintaining them.
Subsequently, much of the work performed on linacs takes place after hours, on nights and weekends. Second devices can serve as backups to help the situation, but they may have to run additional hours to get all patients in. “We’re fortunate because we have multiple [linacs]. So when a machine goes down, patients can be treated through extended hours on other machines,” DiVita says. However, because some of the devices have specific uses, such as the tomotherapy system in the URMC inventory, this is not always possible and uptime becomes key.
Taking Service In-house
The question of uptime or, rather, downtime, will impact whether an in-house program is a cost-effective move. While a small inventory logically suggests contract service, if the location is rural enough that significant downtime results with small problems, it may be cost-effective to develop in-house expertise, whether dedicated or shared. The URMC team handles linacs at campus facilities as well as systems at associate institutions, such as Rochester’s Highland Hospital, Park Ridge Hospital, and FF Thompson Hospital.
URMC first began its in-house program in the 1980s, when its linac inventory was one machine. The local manufacturer service representative was located in Pittsburgh, a 51/2-hour trip by car or plane, according to DiVita.
“If somebody dropped a hand control, the rep would have to hop a plane from Pittsburgh,” Vidro says. “Patients would be canceled from 8 to 12. The rep would arrive by 11 and spend 5 minutes fixing it, and the system would be back online for the afternoon. But when this happened three or four times a week, it got be to problematic.”
Bringing service in-house had an immediate impact on instrument uptime and, ultimately, patient care. The URMC clinical engineering staff knowledge and expertise increased with time and linac acquisitions, and the team was able to handle an increasing number of problems in-house. They now manage approximately 99% of problems with in-house labor and no service contracts. Occasionally, manufacturer input is obtained by phone.
The University of Vermont’s ITS was also driven to provide in-house service because of its out-of-the-way location. “We aren’t in a big urban center, so it takes a while for the manufacturer to get here,” Elliott says. “We can keep the system uptime a lot higher by responding to problems without having to wait for the manufacturer to come in.”
Similarly, institutions with a large inventory will also see immediate economic reasons for investing in an in-house linac service and maintenance program. But the numbers should be run carefully and take into account all costs, not just acquisition capital or training expense. DiVita estimates the cost of the machines falls between $1 million and $3 million, depending on features and applications.
The cost for labor is likely to be expensive. Because the machines are so busy and work is done off-hours, the engineers servicing the machines, who are already some of the highest paid in the department, will cost even more money, with time-and-a-half regulations in place. Problems can take 15 minutes or hours to resolve; PMs will definitely require hours. “The majority of the imaging engineering team’s overtime is spent on linacs, so it’s a very expensive proposition,” DiVita says.
Parts add additional cost, whether purchased as needed (in which case, there is the economic hardship associated with downtime) or kept on hand. Some manufacturers will provide each machine with a parts kit that typically includes many of the system boards. Over time, biomeds will learn which parts are the most useful to have in stock and, with acquisition, more parts are accumulated.
“If you’re able to stock a lot of parts, it will help you in the long run,” Wallace says, acknowledging that not all facilities may choose to make the investment. Spare parts inventories can run into the six figures but can be worth it with multiple linacs.
“The more accelerators you have, the more it makes sense to have extended spare parts because you have more targets where you can use them,” Perec says. If you just have one piece of equipment, you may invest a lot of money into parts that may sit there for the life of the machine.”
Similarly, with one linac to maintain, a biomed may not be able to obtain enough experience to provide the value needed to balance the investment. “An engineer that wants to learn accelerators in a one-system hospital may not have enough exposure to breakdowns to develop the necessary expertise, and it may take him a long time,” Perec says.
For St Vincent Hospital, the associated costs have been worth the money invested. “Once we have removed our last contract in 2012, we will actually save $475,440 annually on service contracts,” Wallace says of the institution’s in-house linac program.
The numbers have contributed to administrative support of the program and should be an approach for anyone who wants to initiate one. “You have to prove to your physicians, who pay the money for the contract, that you can do it better and faster than the vendor. Otherwise there is no point,” DiVita says. Because, again, linacs are complex, expensive devices that need to stay active, useful, and efficient.
Renee Diiulio is a contributing writer for 24×7. For more information, contact .