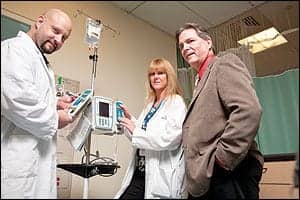
L-R: Biomedical Technician Jim Rominger; Carol Garibaldi, CBET; and Paul Kelley, CBET, director, biomedical engineering and green initiative.
Try as he might, Paul Kelley, CBET, could not avoid winning the award he helped create. The 31-year biomed veteran earned the 2010 California Medical Instrumentation Association (CMIA) Welch Allyn Professional of the Year award during the 1 year he was not on the board—and thus eligible to receive the honor.
While he appreciates the accolades, the director of biomedical engineering and green initiative at Washington Hospital Healthcare System (WHHS), Fremont, Calif, takes pains to deflect glory to the five members of his acclaimed team, which includes four techs and a part-time executive assistant, Fe Mendoza. In a facility with 357 beds and 3,700 pieces of equipment, WHHS is in the same boat as much of the biomed world as it attempts to do more with less.
Having had one employee—Christopher M. Ney, CBET—leave the fold in August 2009 for a 1-year Army Reserve stint in Kosovo (see sidebar), Kelley relies more than ever on the expertise and professionalism of his colleagues. With new projects planned and manufacturer recalls continuing to pile up in 2010, Kelley is grateful for his employees’ experience and is confident in their abilities to do their jobs.
“The thing that I think anybody dislikes is to have somebody over your shoulder telling you what to do every day,” Kelley says. “I hire people who I think are competent and very good at what they do—I can rely on them. My style is pretty much to give them a goal line, give them a deadline, and ask them to get it done.”

L-R: Paul Kelley, Carol Garibaldi, and Jim Rominger review data downloaded from wireless infusion pumps.
Speaking from a perspective of more than 3 decades in the business, Kelley says recalls among manufacturers big and small have never been more prevalent. Whether it is a lack of testing, or pressure to get products on the market more quickly, the recalls have created headaches for biomeds across the country.
To keep up with manufacturer and FDA notices, team members check a national tracking service every Friday that includes an e-mail list of all recalled equipment. Each affected unit is logged into a system that generates work orders. Beyond these formal procedures, staff members have cultivated an elevated awareness when it comes to recalls.
Carol Garibaldi, CBET, says one recent recall on power cord caps affected three different manufacturers. Garibaldi, who serves as lead biomedical technician, reports that when she and staff members first heard about the problem, it required a coordinated response to ensure all bases were covered.
“Although we check electrical safety cords during inspections, we now have to start being extra diligent in looking for these particular cord caps, and we have been working with vendors to decide what is going to be done,” Garibaldi says. “Since the recall actually came from the manufacturer of the power cord, the other manufacturers that use the power cord are not all acknowledging the problem just yet.”
One vendor with detachable power cords readily agreed to send the required 34 new cords, but another took its time before deciding to replace more than 100 units. “A good part of every day is spent dealing with recalls, in addition to all our other work,” Garibaldi says. “Every day, every single day we deal with it. We have added a checkbox on our PM inspections to make sure our data entry clerk does not close any paperwork unless we have noted that we have checked and inspected these and whether or not they have passed inspection. We have implemented a lot of things now to make sure this doesn’t get missed.”
One good bit of news is that most of the recalls do not require that devices be removed from service immediately. Instead, most are the type that should be fixed and/or replaced as soon as possible. Because of this, it is rare that the department must pull things from use prior to repairing.
More than 350 infusion pumps have also been subjected to multiple recalls. When repairs happen, they require a lot of documentation on the part of the biomed team, in addition to the arduous task of rounding up the equipment.
Kelley and the team are able to achieve what can only be described as spectacular results while implementing a patient-centric philosophy. Since Kelley hired all his biomeds, he does not micromanage. Instead, he opts to give his employees the autonomy they have earned.
“He gives us a long leash, because he realizes that we have all been in the field for 10-plus years,” says Biomedical Technician Nick Hillis, CBET. “We like to think that we know what we are doing, and he gives us that leash to take initiative and solve things on our own. At the same time, he won’t let us hang ourselves with that leash, and he is not afraid to step in and give us advice. If he notices that we are struggling, he’ll put his two cents in and get us back on track.”
Thinking Ahead
With efficiency at a premium, the department is preparing for radio frequency identification (RFID) as a way to track equipment and improve patient satisfaction. Within the framework of updating systems and setting the stage for RFID, Kelley has yet another opportunity to use his nonlinear thought processes to achieve a technical goal. “If you stagger access points properly, instead of just putting them straight down the hall, you can use triangulation,” Kelley explains. “So we staggered them into patient rooms, zigzagging down the hallway.” Although no time line has been set for RFID implementation, in the future those access points will help the team locate equipment, according to Kelley.
Another facet of a planned wireless network is split into two phases, with one element acting as a guest network so patients can have Wi-Fi in waiting rooms, lobbies, and even their rooms. At least for this, the tech support will be contracted out, because biomed and IT are busy enough.
“We are looking at moving our infusion pumps on to the second part of the network,” Kelley says. “We are looking at a bunch of different technologies, and of course we don’t want to fill up the whole bandwidth. Initially, we are looking at moving our infusion pumps on to the network so that we can collect the CQI data from our pumps and quickly upload the data sets and pharmacy libraries.”
Telemetry devices will be the next likely candidates after the pumps to move onto the proposed network, and everything will be integrated with a new electronic medical record (EMR) system. “The EMR will require nursing to have some portable devices,” Kelley says. “We are also looking at wireless temperature monitoring for refrigerators and freezers in the pharmacy, the laboratory, and in food service—because a lot of those different departments can be successfully monitored remotely through a wireless network.”
The Green Team

Carol Garibaldi and Jim Rominger inspect failed cord caps from recalled power cords
Paul Kelley has held many titles in his career, including a number of CMIA and American Association of Medical Instrumentation senior positions. In a sign of burgeoning environmental awareness, Kelley has also added green team chairperson to his resume, a position that reflects the growing hospital sustainability movement. “I am willing to bet I am the only biomed in the country with the green team chairperson title,” Kelley says. “I was appointed to lead a high-profile task force, and eventually in 2007 I went to a medical equipment and electronic waste workshop. When I came back, I happened to talk to the CEO. Shortly after that, she announced our hospital green initiative in 2007 as one part of the institutional agenda. I ended up heading that initiative.”
Kelley sought out training from a group called Practice Green Health, an organization that taught him about recycling, energy, water, and even elements such as purchasing. “There is a process called environmentally preferred purchasing where you don’t only look at the cost of the device, but you look at where it was created, how it was shipped, and what you are going to do with it at the end of its life,” Kelley explains. “So you look at the whole life of that device before you make your decision.”
In the couple of years that Kelley has headed the initiative, the program has grown to 25 members representing everything from environmental service and facilities to IT and finance. If departments have old circuit boards, probes, or lead wires, an e-steward company takes care of the hospital’s e-waste recycling, where copper, gold, and other metals get reused.
Staff members such as Jim Rominger, biomedical technician, are now used to tossing materials in the recycle pile. “I don’t find it annoying at all,” Rominger says. “There used to be a lot of times where I would have a part and think, ‘Where am I going to throw this away? Do I put it in the garbage? Now the e-waste company picks up the waste, and it is good to know that it is not being thrown in a landfill.”
Full Tilt

Carol Garibaldi and Jim Rominger inspect a power cord involved in recent recalls.
With five people working at full capacity, something has got to give. Since patient care can never be in jeopardy, the one benefit that has fallen by the wayside is additional training. While everyone is fully qualified to maintain and repair the current equipment, those hoping to expand to other areas have had to wait. The situation is incredibly common, and WHHS has not been immune. “I try to send people to two classes a year, but sometimes, like this year, I haven’t been able to send anybody with Chris Ney gone,” Kelley says. “His absence impacts everybody, but I am always working to improve that training situation.”
As it is, in-house biomeds cover a little more than 50% of the total load, with the remaining percentage under contract with various OEMs. Washington biomeds do not work on equipment for radiology, anesthesia, the larger laboratory units, or the sterilizers. A few independent service organizations pick up the slack.
“We have also had some temporary help while Chris Ney has been gone, because our workload constantly in-creases,” Garibaldi says. “We do a good job in keeping up with it, but it is hectic and we must move fast. At the same time, you have to pay attention to the details and try not to miss things. We look forward to Chris coming back and taking some of this load back off of us.”
|
Read past department profiles in the archives. |
When Ney does get back from Kosovo, the biomeds at WHHS may take the opportunity to bring out a training wish list. For Hillis, an anesthesia OEM school stands at the top of the list. Garibaldi also admits that anesthesia is something she wishes to tackle. If that sounds like a potential conflict, there is no need to fear. Quite simply, the level of mutual respect in the department precludes any such petty disagreements.
“We realize that we are not going to get anywhere if we are fighting with each other,” Garibaldi says. “In the end, we are all here to do a job, and it is so much easier to work with each other.”
Greg Thompson is a contributing writer for 24×7. For more information, contact .
One Man Down—For Now

Christopher M. Ney, CBET, in Kosovo.
It has been more than a decade since the Kosovo conflict ended, but Washington Hospital Healthcare System’s (WHHS) own Christopher M. Ney, CBET, has been doing his part to support America’s continuing presence in the European nation. As a member of the US Army Reserves, Ney is a clinical engineer and noncommissioned officer in charge, which is essentially the military equivalent of a medical maintenance shop supervisor.
While Ney has been in Kosovo since October 2009, his absence began in August of last year when he reported to Georgia’s Fort Benning for soldier skills before moving on to Indiana’s Camp Atterbury for tactical training.
Ney works with one other biomed in Kosovo (a beginner), and he admits that the arrangement differs greatly from the knowledge and equipment resources he had back in California. “At Washington Hospital, I am collaborating with peers, but here in Kosovo I am the supervisor and mentor,” Ney says. “The impact of our department is greatly magnified here, because if one major piece of equipment is inoperable then the ability of the hospital to perform its mission is severely degraded. We do not have the luxury of getting an OEM technician or parts here overnight, so for the most part we repair and maintain everything ourselves with minimal support.”
Ensuring operators know how to properly use equipment, plus regular contact with senior leaders, is an extra overseas duty that is not necessarily commonplace in the States. “This overall experience will be useful for me in regard to promoting and advertising the importance of our department, teaching personnel, and improving time management skills,” Ney adds.

As a member of the US Army Reserves, Christopher M. Ney, CBET, has been serving in Kosovo since October 2009.
Getting married and buying a new home just prior to deployment made the Kosovo trip even more difficult, and Ney admits to some separation anxiety as a result. With a return to America now so close, that anxiety has transformed to anticipation. In addition to seeing his wife and getting back to life in the States, lightening the load for the biomed department will be another added bonus. “I know that my colleagues have continued to provide quality service to our hospital in my absence,” Ney says. “I’m looking forward to further enhancing our effectiveness and strengthening our already strong reputation as a vital department.”
For the biomeds who picked up the slack during Ney’s absence, it has not been easy. However, Carol Garibaldi, CBET, lead biomedical technician at WHHS, believes lessons learned will only help the team as a whole when Ney returns. “The rest of the team has really worked extra hard these past few months, and I think we have grown as a department and learned the importance of being able to rely on each other’s expertise,” she says. “It certainly makes for a better work environment when you have a team who is willing to work for the end cause—which is to make the equipment at Washington Hospital as safe as possible.”
—GT